Reducing waiting times from referral to assessment for routine community CYP mental health services
11 May 2026
Hertfordshire Partnership University NHS Foundation Trust identified a significant backlog in the number of young people waiting over 28 days for assessment on their pathway for routine referrals.
Mental health
Background
Hertfordshire Partnership University NHS Foundation Trust (HPFT) identified a significant backlog in the number of children and young people waiting over 28 days for assessment on their community children and young people’s mental health pathway for routine referrals.
They manage their community children and young people’s (CYP) mental health teams as a quadrant model, with four teams across the county. The trust had been using the Choice and Partnership Approach (CAPA) model, for quite a long period of time. CAPA is a well-known service transformation model informed by demand and capacity theory and can help reduce waiting times in CYP mental health services.
Despite this, services in three of their four quadrants were not performing well. Overall, and particularly since 2020, they had accumulated long waiting lists of about 100 days plus for those referred for assessment on their community children and young people’s mental health pathway and were 50% compliant with CYP being assessed with 28 days. This is against their local commissioning standard of 28 days which is in keeping with the proposed national waiting time standard for access to the community children and young people’s mental health pathway.
Aim
Hertfordshire Partnership University NHS Foundation Trust used data to analyse and understand the cause of the backlog.
The trust aimed to reduce the waiting list for initial assessments for the CYP community pathway and become 100% compliant for children and young people being assessed with 28 days and maintain that level, as well as reducing the number of children and young people waiting for treatment.
Method/Framework
Hertfordshire Partnership University NHS Foundation Trust did not use a formal organisational development methodology to address this issue; instead, they improved their existing operational processes, addressed staffing issues, and standardised ways of working across their four teams.
Their work to reduce CYP community mental health waiting times consisted of four strands:
1) Data
Community Mental Health Team managers worked with the Trust’s Performance Improvement Team to help them understand demand and flow through the service. This enabled them to understand where patients were across the whole pathway – from referral, to assessment, to treatment – as well as how much capacity they had to meet this demand. This work gave them oversight of the entire pathway across all four community CYP mental health teams, and the data helped them to monitor their KPIs and improve service performance.
They held weekly, and sometimes daily, oversight meetings, alongside executive-level oversight, to discuss and monitor waiting numbers and ensure visibility of where patients were on the pathway across all teams. This process continued over two years and, as they began to unpick variation across teams and address staff vacancies, things initially appeared to worsen before improving. This was likely due to a better understanding of the data. It took time to address data quality issues and to understand the true waiting list; once they had improved visibility of the data, they were better able to understand and address the underlying problems.
2) Staffing issues
The Trust had to manage significant staffing challenges, with one community CYP mental health team experiencing a vacancy rate of 50–60% at one point. During the recovery period, they deployed a significant number of agency staff, but have since recruited permanently into these roles, which has made a substantial difference.
They identified a need for staff training in the CAPA model and therefore returned to basics in managing flow and appointments in a more structured way. The most significant improvement came from redeploying staff and appointing the service manager from the higher-performing team to oversee the entire pathway across the county. This enabled a single standardised approach, rather than four different ones.
3) Changes in how they work
There has been a cultural shift, with teams now working collaboratively across the four services rather than in silos. One manager now oversees the whole pathway. Joint training sessions are run across teams, with regular meetings to discuss pathways and processes.
They also undertook a large piece of work to understand capacity and demand, as there had previously been no clear mechanism to review capacity and allocate cases effectively. The Performance Improvement Team supported this work. Data was used to identify anomalies in demand and flow across the pathway, enabling the teams to understand these patterns rather than make assumptions about their causes. This challenged long-standing beliefs about the service and how it operated. Assumptions are now revisited as circumstances change.
Standardised job plans have been implemented across the service for all professions and reviewed in relation to the complexity of the CYP cases being seen. The teams reviewed the average number of sessions provided and built a complexity scale into the job plans to provide greater flexibility. In addition, quarterly reviews are now undertaken with each clinician to review caseloads and agree what is manageable. This represents a significant change in how some teams operate.
Clinical staff are now undertaking a set number of initial assessments, depending on their hours and responsibilities. There is now greater consistency and a more equitable distribution of assessment activity across clinicians.
4) Working in a more standardised way
Initially, there was uncertainty about whether the CAPA model remained appropriate. CAPA was found to be more firmly embedded in some teams than others; where it was implemented, it was working well from a capacity and demand perspective. The Trust has since decided to retain the CAPA model, developing it to better suit their needs. It has now been embedded across all four teams, with improved performance outcomes observed.
Team managers have reviewed and standardised their processes. The operational policy for CAPA was reviewed, and the Trust has completely rewritten the operational policy for the service. The most significant change relates to how referrals are managed and prioritised, and how clinicians’ time is allocated. While these principles already existed within CAPA, the teams have now agreed a clear set of working principles and are actively implementing them in practice.
Results
The Trust are now about 100% compliant for the number of CYP being assessed on the community mental health pathway within 28 days.
- Graph 1 below shows how the number of CYP being seen within 28 days increased to 86% in January 2026.
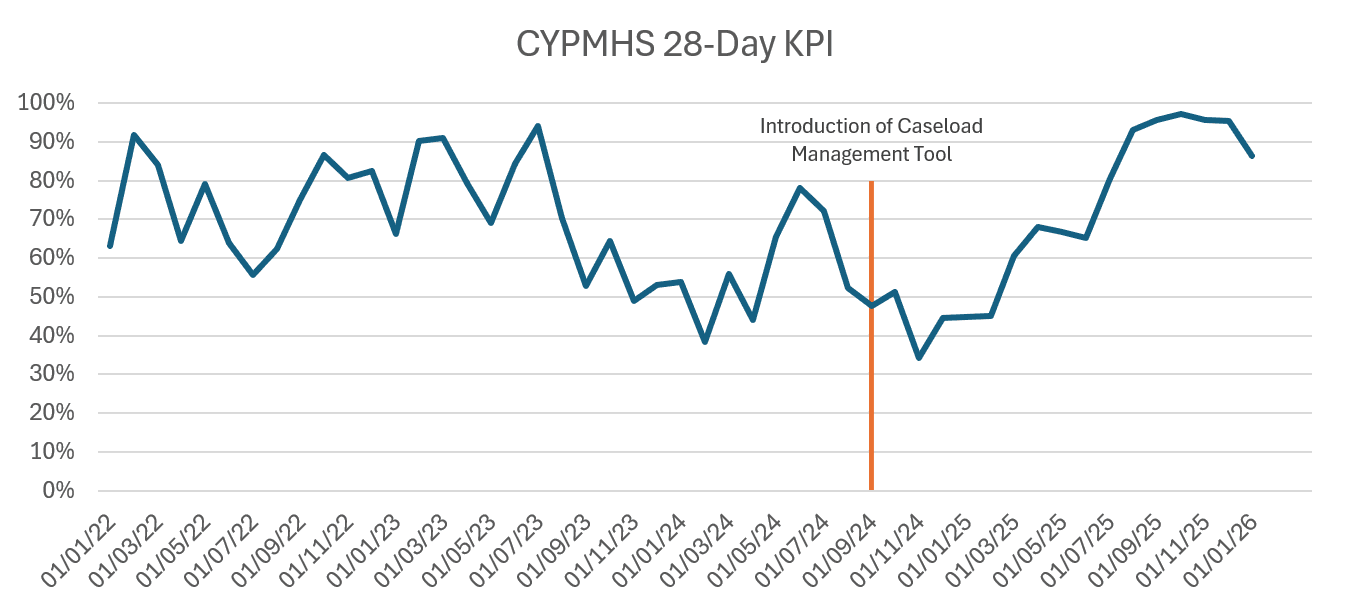
-
Graph 2 below illustrates how they reduced the number of days waiting by 66 days since 2022.
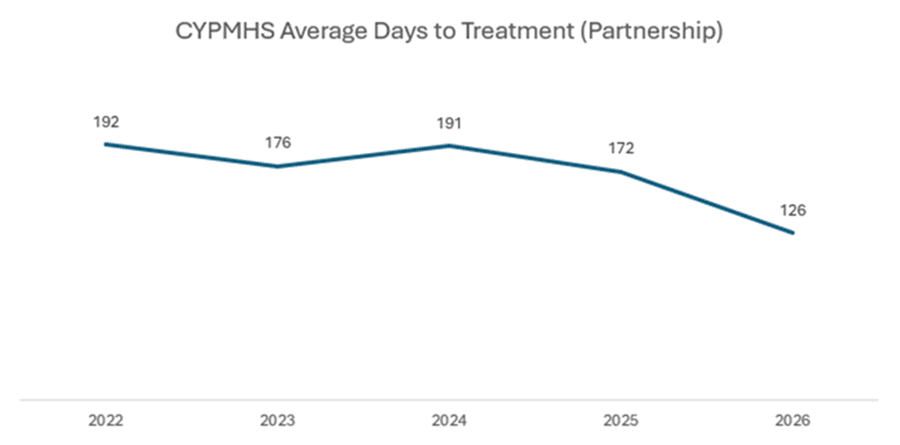
-
Graphs 3 shows that the number of children and young people entering treatment with 2 or more contacts, has increased to 1,693 in February 2026 compared to 1,547 in September 2024.
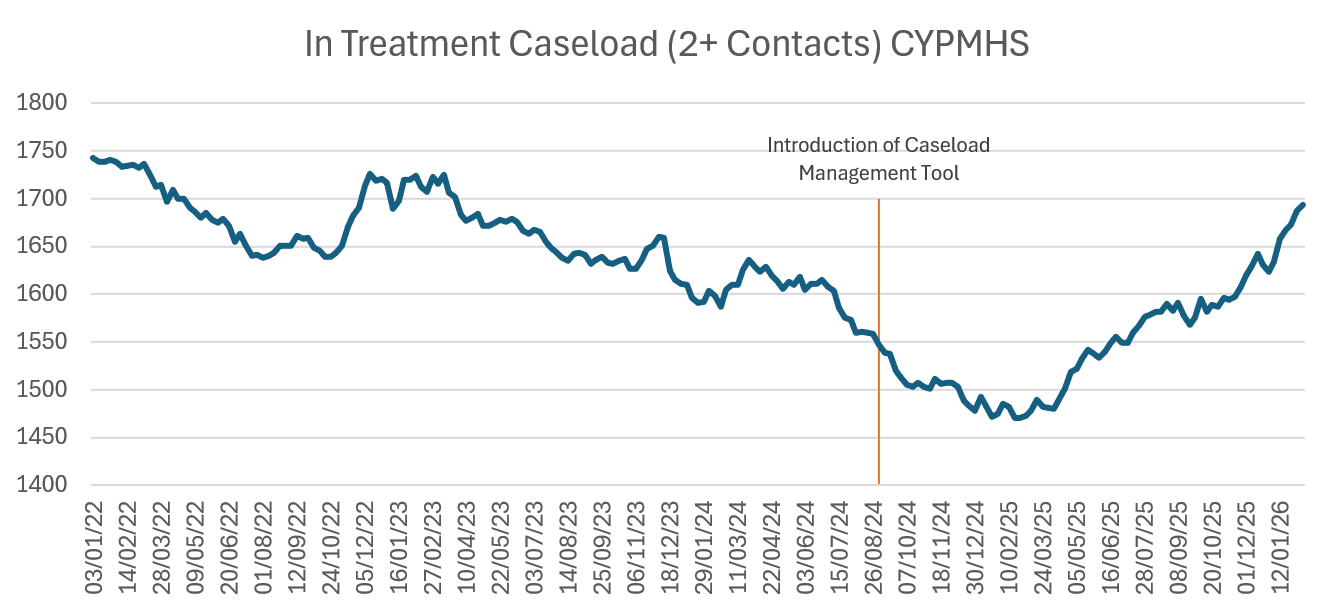
Lessons learned
-
Using data and having oversight of the whole pathway as part of good operational management of the service, to understand numbers waiting and where they are on the pathway.
-
The overall service manager working really closely and collaboratively with the four quadrant managers, so they had one standardised approach.
-
Revising the CAPA model to meet current needs, implementing it across the four teams and ensuring that staff are trained in the model.
-
Working in a more standardised way across the four teams in terms of how they operate, and how they understand capacity and flow.
Next steps
-
Continuing to use data as a whole team to understand demand, flow and capacity, as well as identifying opportunities to improve practice.
-
Working on how to sustain 100% compliance and manage any surges in demand.
-
Maintaining quality of care whilst increasing the number of children and young people using and flowing through their services.
-
Supporting staff wellbeing to ensure they feel motivated and committed to the work, and that they have the right skills for the job.
IMPACT summary
Hertfordshire Partnership University NHS Foundation Trust used data to understand their long waiting times for assessments in their community CYP mental health teams and were persistent in monitoring progress towards becoming 100% compliant and significantly reducing their waiting lists. The trust has used the CAPA model for many years, and rather than looking for a new model, they evaluated how they used CAPA and updated it to meet current needs. They worked hard to implement changes in the way the team worked from an operational perspective, so they had a better understanding of capacity within the team, and flow through the service. They addressed staffing issues such as high vacancy rates within the teams and put one manager in charge of the whole pathway.
Contact details
For more information about the work in this case study, contact Fiona McMillan-Shields, divisional director for specialist services at Hertfordshire Partnership NHS Foundation Trust, at fiona.mcmillan-shields@nhs.net.